The HbA1c Number That Could Add Years to Your Life
Your doctor says your blood sugar is "normal." But science says normal isn't optimal — and the gap between the two might be decades of healthy life.
BIOMARKERS
5/13/20263 min read
Hemoglobin A1c (HbA1c) is one of the most powerful single numbers in preventive medicine. It tells you — with a single blood draw — the average glucose that has been flowing through your body for the past 60–90 days. And according to a growing body of peer-reviewed evidence, where you sit on that scale doesn't just define whether you have diabetes. It may define how long, and how well, you live.
What HbA1c Actually Measures
Glucose binds irreversibly to hemoglobin inside red blood cells — a process called glycation. Because red blood cells live roughly 90–120 days, the percentage of glycated hemoglobin at any moment reflects your sustained glucose exposure over the prior three months. This is why HbA1c is far more informative than a fasting glucose snapshot: it cannot be gamed by skipping breakfast the morning of your test.
The Research Is Unambiguous: Lower Is Better (Down to a Point)
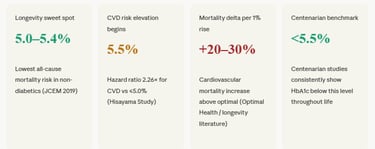
The Journal of Clinical Endocrinology & Metabolism published a landmark prospective cohort analysis of 15,869 participants from the Health and Retirement Study. The finding was striking among people without diabetes, those with an HbA1c of 5.4% had the lowest risk of all-cause mortality. Risk rose in a reverse J-shape — increasing both below 5.0% and with any sustained elevation above the optimal band.
"In participants without diabetes, those with an HbA1c level of 5.4% were at the lowest risk of all-cause mortality. The corresponding optimal range for overall survival is predicted to be 5.0–6.5%."— Journal of Clinical Endocrinology & Metabolism, 2019 (Oxford Academic)"
A 2024 study in Scientific Reports (Nature Publishing Group) reinforced this picture, documenting a U-shaped association between HbA1c and all-cause mortality in cardiovascular disease patients — an echo seen across multiple populations worldwide.
An independent meta-analysis across six European and US cohort studies (28,681 non-diabetic participants, mean follow-up 10.7 years) found that elevated HbA1c above 6.0% — still below the diabetes threshold — was associated with a 14–19% increase in all-cause mortality and cardiovascular events, even after adjustment for traditional risk factors.
Cardiovascular Risk: It Starts Earlier Than You Think
The Hisayama Study, a prospective 7-year community cohort of 2,851 Japanese adults, stratified participants by HbA1c and tracked cardiovascular events. The result was sobering for anyone in the "technically normal" range: subjects with HbA1c of 5.5–6.4% had a 2.26-fold higher risk of cardiovascular disease compared with those at or below 5.0%. Those at 6.5% and above faced a 4.43-fold increased risk. The message: the cardiovascular damage clock starts ticking well before a diabetes diagnosis.
Brain Health: HbA1c and the Dementia Connection
The cognitive consequences of chronically elevated glucose are increasingly well-documented. A 2024 study in Alzheimer's & Dementia linked HbA1c variability in type 2 diabetes patients directly to elevated dementia risk — with both vascular and neurodegenerative pathways implicated. High glucose damages the microvasculature that feeds the brain, promotes neuroinflammation, and accelerates the formation of advanced glycation end-products (AGEs) in neural tissue.
The mechanism is glycation itself. When excess glucose binds to proteins — including those in the brain's blood vessels and neuronal membranes — it creates AGEs: molecular cross-links that stiffen tissue, impair cellular function, and fuel inflammatory cascades. Reduced dietary AGE intake has been shown in randomized controlled trials to meaningfully lower circulating AGE levels, suggesting that what you eat matters as much as how much sugar you consume.
Why "Within Normal Range" Is the Wrong Goal
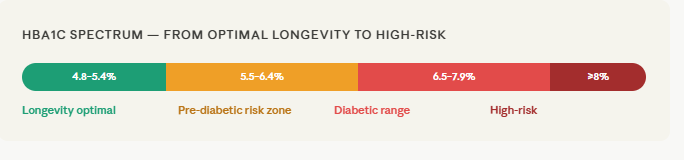
Standard clinical thresholds classify HbA1c below 5.7% as "normal," 5.7–6.4% as prediabetic, and 6.5% and above as diabetic. These are diagnostic categories, not longevity targets. The research reviewed above consistently places the biological optimum at 4.8–5.4% — a range that most adults in developed countries do not inhabit, given the modern diet.
For longevity optimization, aiming for the diagnostic "normal" is like setting your car's oil change interval to the manufacturer's minimum and wondering why the engine ages prematurely. The goal isn't to avoid disease labels — it's to maintain the metabolic environment in which your cells thrive.
The Bottom Line
HbA1c is not just a diabetes test. It is a continuous biomarker of metabolic stress, vascular aging, and inflammatory load — one that predicts cardiovascular disease, cognitive decline, and all-cause mortality across its full range, not just above the diabetes threshold. The science is consistent: an HbA1c of 5.0–5.4% is the longevity sweet spot. Getting there — and staying there — is one of the highest-leverage interventions available to anyone serious about adding healthy years to their life.
The tools are not exotic: diet quality, movement timing, sleep, and resistance training are sufficient for most people to move the needle meaningfully within three months. Your next HbA1c result is a 90-day report card on your metabolic environment. Make it count.


Insights
Expert guidance for health-conscious professionals.
Support
Connect
info@genthealthhub.com
© 2025. All rights reserved.
